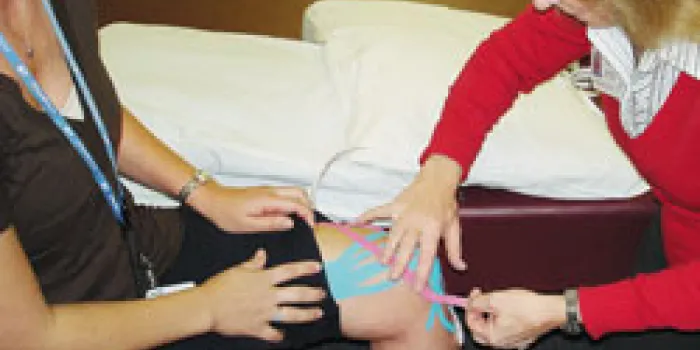
Observant fans detected something different about some athletes competing in the 2008 Summer Olympics in Beijing, China—strips of tape draped across their shoulders, down their thighs and on their shins. Kinesio taping, while new to the Olympics, has been used for more than 25 years for athletes and people in the bleeding disorders community.
“With hemophilia patients, it’s tremendously useful because it helps with edema, or swelling, by draining the excess fluid and getting the blood out,” says Cindy Bailey, PT, DPT, OCS, SCS, director of the physical therapy program at the Hemophilia Treatment Center at Orthopaedic Hospital of Los Angeles. She has co-taught kinesio taping seminars for the past 12 years and conducted a hands-on session for physical therapists at the National Hemophilia Foundation’s 57th Annual Meeting in San Diego in 2005.
Bailey uses the tape for patients with joint bleeds, soft tissue bleeds or injuries. She also uses it in patients after shoulder, knee and elbow repair or replacements.
The 2-inch-wide tape is made of an elastic, latex-free cotton fabric that is the same thickness as the epidermis, the skin’s outer layer, and imitates its properties. It comes in a variety of colors from hot pink and aqua to black. It is named for its kinesthetic, or movement, ability; it stretches 30% to 40% beyond its original length. Kinesio tape sticks to the skin via a heat-sensitive adhesive, which may secure it for up to five to 10 days. The patient’s body heat improves the tape’s adhesion. In addition, patients can shower and swim in it.
Taping techniques vary, depending on where the tape is placed and why. For sprains and strains, strips of tape are used. For joint bleeds and swelling, a more elaborate design is created. “It looks like an octopus with five or six skinny legs going across the knee, elbow, thigh or whatever joint you’re taping,” says Bailey. To stretch it or not to stretch it depends on several factors. “For edema taping, there is no stretch on the tape,” Bailey says. “If it’s over a joint, you place the joint through its available pain-free range of motion, then place the tape on.”
When a patient goes about daily activities or engages in exercise, the skin moves, causing the tape to create a gentle massaging motion. The tape microscopically lifts the skin, allowing body fluids in the injured area beneath it to flow again, improving circulation and reducing edema, inflammation and pain.
PTs aren’t the only ones learning the taping techniques, however. Bailey’s rule of thumb is, “If they can reach it, they can tape it.” By the third session, most of her patients can do their own taping.
The tape can be adjusted during follow-up physical therapy sessions. “Once the swelling subsides, I take the tape off, take the patient to their new available pain-free range of motion and put another taping technique on,” Bailey says.
The taping technique can be used alone or as an adjunct to other treatments in bleeding disorders patients. In children, for instance, a recent bleed might require a brief period—24 to 48 hours—of splinting and taping. “The tape allows them to get the blood out faster and reduce the swelling quicker, so we can start range of motion sooner.”
Although Bailey knows of no long-term studies of the tape’s effectiveness in bleeding disorders patients, she has seen its benefits firsthand. “If we can get the tape on within 24 hours after surgery, it makes the postsurgical bleeding and edema much less of a factor in their rehab,” says Bailey. “For hemophilia patients, it has truly changed the amount of time they have their joints immobilized.” That translates into added dividends down the line—healthier cartilage and increased range of motion ensure better joint health in the future.