Read more about the D'Ambrosios in stepmom Cheryl's own words, in our Community Voices section.
A hangnail hardly constitutes a medical crisis. But it could have provided a clue.
Thirty years ago, when Teresa D’Ambrosio was a newborn, she had a hangnail that kept bleeding. Her parents called the pediatrician, but he wasn’t concerned. A month later, flulike symptoms and seizures landed Teresa in the hospital. She had an intracranial hemorrhage, or bleeding in the brain.
Tests revealed that Teresa had factor V deficiency, a rare inherited bleeding disorder. The incidence of FV deficiency is estimated at one in 1 million, with fewer than 200 known cases worldwide.
People with FV deficiency provide a challenge to their treaters. There is no factor concentrate they can infuse at home. They can have an array of symptoms, not necessarily correlated with the amount of factor in the blood. Further, difficult bleeds can result in lengthy hospital stays. Although treating can be tricky, some standard protocols and precautions help improve patients’ quality of life.
Form and Function
During the clotting cascade, FV converts the plasma protein prothrombin to thrombin, the first step in clot formation. The clotting protein is found in plasma and platelets, so it can affect both bleeding and clotting.
FV deficiency is caused by a hereditary condition that results from genetic mutations on chromosome 1. It was first identified in a Norwegian woman in the early 1940s and occurs as often in men as in women. Symptoms of FV deficiency can be similar to hemophilia, hence the alternate name parahemophilia. “While patients can have joint and muscle bleeds, as in hemophilia, they are more likely to have mucosal, umbilical cord and intracranial bleeding. Some FV deficient patients will have bleeding at birth,” says James Huang, MD, director of pediatric hematology at University of California, San Francisco Children’s Hospital.
Teresa’s severe FV deficiency resulted in a bevy of bleeds. “I had a lot of nosebleeds, teeth bleeds and gum bleeds,” says the Mercer Island, Washington, woman. After the initial intracranial hemorrhage, she developed a blood clot in her brain. A neurosurgeon operated to remove it, drain the blood and insert a shunt. Although developmentally delayed as a result, Teresa is active in her community. “I’ve worked at Starbucks for nine years as a busser,” she says. Teresa volunteers at the local Boys and Girls Club. “I clean up after the kids. They’re very messy,” she says, laughing.
Over the years, Teresa has been hospitalized for up to one month for bleeds in her head, shoulder and abdomen, as well as between vertebrae and surrounding her liver. A port, implanted when she was a teenager and recently replaced, helps with the many transfusions she has been given.
Teresa’s younger sister, who also has FV deficiency, has had her share of bleeds, too. “The biggest problem was muscle bleeds and joint bleeds from being an active child,” says the 27-year-old, who works at an architectural firm. Being competitive didn’t help, says Cheryl, the sisters’ stepmother. “During group swimming lessons, she wanted to be the first one across the pool.” That would invariably lead to a leg bleed. “She would miss every other class because we were taking her in for fresh frozen plasma (FFP),” says Cheryl, 57, a process developer and project manager at an aerospace company. Cheryl married the girls’ father, Tony, a widower, when the girls were 11 and 14.
Joint bleeds affected Teresa's sister physically and socially. “I do remember feeling embarrassed at school because I was limping or I had a hurt arm. A lot of times my legs would look pretty scary because I had a lot of bruising on them.” A target joint in her right ankle became chronic. “From age 8 to 13, I was injuring it all the time,” she says. “It took me years to get over that one.”
Getting over her menstrual periods was even more difficult. “The second period ended up being really severe.” Weak from the blood loss while on vacation in Missouri, Teresa's sister fainted in her stepmother’s arms. “I ended up in the hospital,” she says.
But severity and symptoms do not always go hand in hand. “Patients with lower levels of FV do tend to bleed more, but patients of all levels have various kinds of bleeding problems,” says Huang. A 2008 literature review by Huang and a colleague revealed that even patients with identical genotypes and very low FV levels (<1% of normal) had marked variation in their symptoms. (See “Learn More” section below.) “With a lot of these rare bleeding disorders, the blood test may not truly reflect what’s going on in the body.”
Treatment
“The current treatment is fresh frozen plasma,” says Huang. “For mucosal bleeding that’s not severe, the antifibrinolytic agents, like aminocaproic acid, can be used. If you have menorrhagia, hormonal therapy might be an adjunct to minimize bleeding.”
For the D’Ambrosios, obtaining FFP was not so straightforward. Even with standing orders to receive it, sometimes the family ran into roadblocks. Once after phoning in the order ahead of time—it takes two hours for the plasma to be secured and thawed—upon arriving at the hospital, the family was told the standing orders had expired. Another time an urgent care physician said, “We’re going to see what’s going on here. We don’t just order blood products.”
The “diagnose first, treat later” philosophy did not sit well with the D’Ambrosios. “We can’t wait six hours for plasma,” says Cheryl's younger stepdaughter. “Cheryl learned quickly to argue with the staff or question procedures to get people to understand that.” Now that the family relies on the Puget Sound Blood Center (PSBC), their hemophilia treatment center (HTC), as the liaison, the process is smoother. “If we do have some negotiations or if the doctor hesitates, we make the HTC intervention call from our cell phone,” says Cheryl. “Once the doctor has spoken directly with the HTC, he or she will say, ‘I’ll order it. I’ll take care of it right away.’”
Plasma Safety
The reticence of some physicians to order FFP is related to safety. Plasma is derived from the pooled blood of donors. “Our blood supply is as safe as it’s ever been, but there still is that possibility of infection and allergic reactions,” Huang says. The causes of such allergies, while not well understood, can be due to the presence of normal blood constituents, he says. “In addition, it is conceivable that donors could passively transfer proteins from food they ate, such as peanuts, to which the recipient may be allergic,” says Huang.
 Mike Murdock/American Red Cross
Mike Murdock/American Red Cross
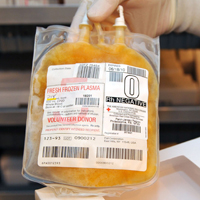
Fresh frozen plasma derives from pooled blood of donors and is used to treat factor V deficiency.
Once Cheryl became involved in her stepdaughters’ medical issues, the D’Ambrosios had to face the plasma dilemma head on. “Do you know what you’re putting into these girls?” Tony, the girls’ father, asked her pointedly. “They could get HIV. They could get hepatitis. They could die from it.” Waiting, however, had its own downside. Instead of two units of FFP at the outset, a delay could create a situation where six units were needed instead. “You do the math and finally change your paradigm,” Cheryl says. “When you nip it in the bud, there are fewer units used and less risk.” Cheryl and Tony now agree on this. Both daughters have experienced occasional itching from mild allergic reactions after FFP treatments. Over-the-counter antihistamines provide relief.
A concern for patients receiving routine transfusions is transfusion-related acute lung injury (TRALI). TRALI occurs in approximately one in 5,000 plasma product transfusions. The symptoms typically appear within six hours of the transfusion and include fever, low blood pressure, fluid in the lungs and severe respiratory distress. “That’s always a possibility when you receive any blood product, but I don’t think there’s a greater risk specific to FV-deficient patients,” says Huang. Patients most at risk are those on weekly prophylactic FFP therapy, he says. Huang is concerned, but says the risk is relatively low. “For a severely affected FV-deficient patient who bleeds often enough to need weekly prophylaxis, that risk translates to roughly one TRALI event in 100 years,” he says.
Some physicians have had success with off-label use of recombinant factor VIIa in treating certain FV-deficient patients. (See “Safe and Effective,” HemAware November/December 2006, p. 43.) Benefits include reduced risk of infection and a lower volume needed per infusion. “We would use it in patients with an inhibitor to FV and in those who are bleeding and not responding to FFP,” Huang says. However, dosage has not been well studied and is, therefore, not standardized. The risk is that too much could lead to excessive blood clotting. Because platelets contain FV, they may be effective in FV-inhibitor patients, says Huang.
Managing Bleeds, Managing Life
Now that she’s an adult, Teresa's sister is managing her life and her bleeds fairly well. “Part of it is understanding what level of shape I need to be in,” she says. She does sit ups, push-ups, some stretching before activities, and lives close enough to walk to work. She also enjoys hiking in the summer. “Using common sense, I can pretty well prevent most joint injuries.”
The longest she has gone without FFP is three months. “I need it about every one to two months,” she says. PSBC has been responsive to her needs. “I can call them any time and they set it up at the center or one of the local hospitals.”
Still, she yearns for the day when she has access to a portable product specific to her condition. “I feel tethered to this one place,” she admits. Traveling or living somewhere else are only dreams. “I’d like to see more attention paid to treatment for the rare blood disorders,” she says. With her stepmother’s advocacy efforts, including the recent publication of Cheryl’s book on FV deficiency, Pooling Blood, and increasing traffic on a Web site Cheryl created, mygirlsblood.com, her dream may be realized sooner than she thinks.

