Unexplained weight loss. Short on stamina. Winded while running. Those symptoms landed David Britton, who has mild hemophilia A, in the emergency room (ER) in 2011. “It was heart failure related to the water I was holding because my kidneys were not working properly,” says the 53-year-old engineer from Harrison Township, Michigan. “They diagnosed me with chronic kidney disease.”
Britton’s kidneys had been compromised by the hepatitis C virus (HCV) he was diagnosed with in 2000. “I have cryoglobulinemia, which attacks the kidneys,” he says. Cryoglobulinemia, the presence of abnormal proteins called cryoglobulins in the blood, is an autoimmune response to long-term chronic infection, such as from HCV. It was responsible for causing Britton’s heart and kidney damage.
Chronic kidney disease often remains undiagnosed for decades because its symptoms develop slowly and can mimic other conditions. Because your kidneys perform many vital functions, it’s important to understand what they do and how to care for them, especially if you have hemophilia, HCV and HIV.
Removing, recycling and regulating
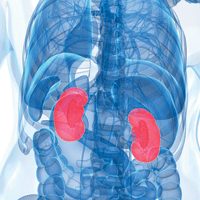
Science Photo Library/Glow Images
The kidneys are paired organs about 4½ inches long and 2½ inches wide. They are located below the rib cage near the middle of your back. They are enclosed by a thin, fibrous capsule and cushioned by a layer of fat. Each kidney contains more than 1 million nephrons, each made up of a glomerulus and tubule. The glomerulus is a cluster of tiny blood vessels, or capillaries, that serve as a filter between the blood and the urine; the tubule is a collecting tube for fluids.
The kidneys remove waste products from the blood; recycle other components to maintain a chemical balance of sodium, potassium, phosphorus and water; and regulate blood pressure and pH. According to the National Kidney Foundation (NKF), 20% of the blood pumped by the heart goes to the kidneys. About 200 quarts of blood undergo a complex filtration system in the glomeruli daily; 198 quarts are returned to the body. The remaining two quarts of water and waste are excreted as urine, which leaves the kidneys via ureters that carry it to the bladder.
Three hormones are produced by the kidneys. Renin helps control blood pressure and keeps electrolytes balanced. Erythropoietin stimulates red blood cell production in the bone marrow. Calcitriol, the active form of vitamin D, helps the body absorb calcium.
Effects of diabetes and hypertension
Chronic kidney disease means the kidneys’ filtration system is broken, allowing waste products and toxins to build up in the body. The majority of causes are from a problematic pair. “In the US, about three-fourths of chronic kidney disease is from long-term complications from uncontrolled diabetes and hypertension,” says Brent Miller, MD, associate professor of medicine in the division of renal diseases at Washington University School of Medicine in St. Louis. It can take decades for kidney disease to progress, he says.
When you have high blood pressure, your heart and kidneys have to work harder. “If you run the oil pressure really high in your car, you’re going to damage certain components,” says Miller. That goes for the kidneys, too. After 20 or 30 years of uncontrolled high blood pressure, the kidneys’ filters are worn out.
High blood pressure is more common in people with hemophilia than in their peers, but it’s not clear why. A 2013 study in Hypertension found that in the more than 450 adults with hemophilia in the study, 49.1% had high blood pressure, compared to 31.7% of the control group. “There may potentially be microbleeds that are occurring in the kidney over time that might damage its ability to control blood pressure normally,” says Patrick F. Fogarty, MD, director of the Penn Comprehensive Hemophilia and Thrombosis Program at the University of Pennsylvania Medical Center in Philadelphia.
Diabetes affects the kidneys by exposing them to high levels of the blood sugar glucose, which are toxic. “It allows all this gunk to be deposited on the filter, which can become fibrosed and destroyed,” says Miller.
Other causes of kidney disease
Igor Grochev/Thinkstock
Long-term viral infections can injure your kidneys. “Both HIV and HCV directly cause kidney disease. They both cause glomerulonephritis (damage to the glomeruli),” says Miller. Exposure to intravenous contrast solution used in imaging tests for HIV and HCV can also be harmful, he cautions. “The iodinated contrast is vasoconstrictive, so it immediately decreases the blood flow to the kidney temporarily.”
The combination of HIV and diabetes can produce an additive effect when it comes to kidney disease, shown in a 2011 study published in PLoS ONE online. More than one-third of those who had diabetes and were HIV-positive had elevated levels of albumin in their urine, an indicator of kidney disease, compared with 13% of those who were HIV-positive and not diabetic. Further, high viral loads also contributed to kidney damage. Those most at risk tended to be older, with blood pressure that wasn’t well controlled.
Further, antiviral drugs can do damage. “Some of the drugs, particularly for HIV, can have some toxicity to the kidneys,” Miller warns. A 2012 study published in the journal AIDS concluded that tenofovir, a common oral antiretroviral drug, could cause irreversible kidney damage in people with HIV/AIDS. The 2011 PLoS ONE study found that exposure to abacavir, an antiretroviral drug, is associated with higher rates of chronic kidney disease and can lead to cardiovascular disease, including heart attacks. Indinavir, a protease inhibitor that blocks HIV replication, can cause kidney stones. (See sidebar, “Kidney Stone Awareness.”)
Over-the-counter medications can also tax the kidneys. Overuse of nonsteroidal anti-inflammatories, such as aspirin and ibuprofen, can be harmful. “But most people with hemophilia are avoiding those because of the bleeding complications,” Miller says. Herbal products should be taken with caution. In 2001, the US Food and Drug Administration warned that Chinese herbs with aristolochic acid, used in dietary supplements, could cause permanent kidney damage. Always consult with a physician prior to taking any herbal medications.
Slow symptoms
The problem with kidney disease is that patients remain asymptomatic for a long time. “It’s not usually something the patient knows about until it has progressed to an advanced stage,” Fogarty says. By then, kidney failure can cause electrolyte imbalances, such as with potassium, which can affect your heart function, he says. Britton’s blood pressure topped out at 180/90, so he was prescribed several medications to lower it. “My liver doctor called me immediately and said, ‘Stop taking those medicines, because your potassium is way out of control.’ ”
Other later-stage symptoms cause everything from urinary tract issues to fatigue. “If you’re losing a lot of protein, your urine might look foamy, like soap suds,” Miller says. Swelling in the hands and feet can occur. “I was retaining water,” says Britton. Some of Miller’s patients start their journey in the ER with flulike symptoms. “That’s when they’ll find out they have kidney failure,” he says. “The symptoms are so insidious.”
Necessary tests
The NKF recommends screening tests for kidney disease. The first is a blood pressure reading. Anything above 120/80 is considered borderline or high, depending on the reading. High blood pressure can be both a cause and effect of kidney disease.
Another test checks the amount of albumin in your urine (proteinuria). “If your filter is damaged, albumin leaks through the glomerulus into the urine,” Miller says. “It’s a marker for damage.”
A third test, the estimated glomerular filtration rate (eGFR), measures the amount of creatinine in your blood, then calculates the amount of kidney function you have. It takes into account your age, gender, height, weight and race. Creatinine is a breakdown product of muscle cells that healthy kidneys filter into the urine. Its presence in the blood, however, is a tip-off of filter malfunction.
“The eGFR is the amount of blood that the kidneys purify every minute in milliliters (ml),” says Miller. There’s a range of normal values, but the average is around 100. “That means you clear 100 ml of blood of all your toxins every minute,” he says.
As chronic kidney disease advances, the eGFR decreases and complications increase. The NKF divides kidney disease into five stages. Stage 1, when your eGFR is 90–100, means you have normal function. Symptoms don’t usually show up until Stage 3, when the eGFR is 30–59. With <60% of kidney function, patients may become anemic. At Stage 5, when the eGFR is <15, you have kidney failure.
Your doctor may order additional tests to evaluate kidney disease. An elevated blood urea nitrogen (BUN) level means the kidneys are not adequately transferring the waste product urea from the blood into the urine. Imaging scans or a biopsy can provide even more information on your kidney health.
Tailored treatment
Seeing a nephrologist, or kidney specialist, is important for kidney care. “If you have signs of progressive kidney disease, combinations of disease states and symptoms, that’s when we want to see you,” says Miller, who is a nephrologist. Such signs include high blood pressure, diabetes, protein in the urine and abnormal creatinine levels. Blood in the urine (hematuria) can be tricky for patients with hemophilia, he notes.
Treatment often begins with lowering your blood pressure. You may be prescribed an angiotensin receptor blocker (ARB) or angiotensin-converting enzyme (ACE) inhibitor, both of which can slow the progression of kidney disease. Or a more conservative approach may be taken. “I have seen patients who were hypertensive lose 20 pounds and no longer be hypertensive,” Fogarty says.
Simple lifestyle changes, such as quitting smoking, engaging in physical activity and eating special diets, can do a great deal to ease the kidney burden. “A low-salt diet and, for those with diabetes, decreasing the carbs and simple sugars,” Miller says. Britton has revamped the foods he eats. “I’m balancing a heart-healthy diet with a low-potassium diet,” he says.
A low-cholesterol diet may be needed as well. Cholesterol can build up on blood vessel walls, bumping up your blood pressure. If you continue to show signs of proteinuria, your doctor may suggest a low-protein diet to take a load off the kidneys.
Keeping kidney failure at bay
All of these measures can help prevent end-stage kidney disease, whose treatment is limited to either dialysis or a kidney transplant. These options are especially difficult in people with hemophilia, because of the added bleeding risk and medication management issues.
Rituximab, a cancer drug that helps combat autoimmune diseases, saved his life, says Britton. It quieted his immune system, and lowered his creatinine and protein levels. He regained his strength, his weight and his well-being. “After the first rituximab treatment, I started doing things in the yard and around my house again,” Britton says. And his blood pressure is now 120/80. “I attribute a lot of that to the treatment I’ve been getting for my kidneys—the rituximab to treat the complications of chronic kidney disease,” he says.
In November 2013, the NKF and the Renal Physicians Association recommended screening of kidney disease for high-risk patients: those who are over 60 and have a family history of kidney failure, and people with high blood pressure, diabetes and from certain ethnic groups, including African-Americans. They also recommended at least annual testing of proteinuria for those with diabetes and high blood pressure.
When it comes to kidney health, communication between your hemophilia treatment center (HTC) and primary care physician (PCP) is crucial. HTCs don’t perform routine urinalysis, says Fogarty. “We expect the PCP would screen for kidney disease in susceptible patients,” he adds. But high blood pressure is another matter. “Because hypertension could be related to underlying diagnosis of hemophilia, and could also be related to changes in kidney function, it’s important for both the PCP and the patient’s HTC doctor to be paying attention to it,” Fogarty says.