It may be small, but it can bring a Navy SEAL to his knees. With its spasms of pain, a kidney stone has a way of grabbing your attention. “When my kidney stone started to move, that was the real pain,” says Zach Marcella, 22, who has severe hemophilia B with an inhibitor. He’s had painful joint bleeds, but this was different. “There was a stabbing, burning sensation as it was coming out—that’s the worst pain,” says the sophomore pursuing a pre-pharmacy degree at Middle Tennessee State University in Murfreesboro.
If you have a bleeding disorder and you’ve had kidney stones or they run in your family, you need to know what to do before you’re headed to the emergency room (ER) doubled over in pain.
Urinary tract 101
Your urinary tract is your body’s disposal system for liquid wastes and water. It is composed of the kidneys, ureters, bladder and urethra. Every day about 200 quarts of blood flow through the kidneys, which then produce about 1–2 quarts of urine. Urine moves through the ureters from each kidney to the bladder, a storage organ. It exits through the urethra.
The who and how of kidney stones
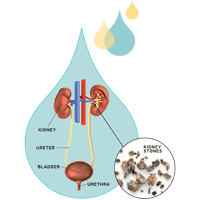
3drenderings/Thinkstock (graphic);
Piotr_Malczyk/Thinkstock (stones)
Kidney stones are common, occurring in about 1 in 10 Americans, says the National Kidney Foundation (NKF). They account for nearly 1 million doctor’s office visits and 300,000 trips to the ER every year, according to the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK).
Men are nearly twice as likely to form a kidney stone as women. Others at risk include those who are obese or who have hyperparathyroidism, overactive parathyroid glands. Inflammatory bowel diseases, such as Crohn’s disease, and hypercalciuria (large amounts of calcium in the urine) also raise the risk.
Many medications are also in the mix. If you frequently take antacids, watch out. Those containing calcium can cause kidney stones. Other culprits include the HIV drug indinavir, and certain diuretics and anticonvulsants.
The series of events leading to a kidney stone starts with dehydration, not drinking enough water. Minerals in the urine then become highly concentrated, forming crystals. When enough crystals clump, they create a stone. The majority of kidney stones in the US contain calcium oxalate, calcium phosphate or both. Others are composed of uric acid or cystine, an amino acid. Struvite stones, made of magnesium and ammonia, tend to develop in women with a kidney infection.
“It’s all a matter of chemistry, of minerals precipitating in your urine,” says nephrologist (kidney specialist) Brent Miller, MD. He is associate professor of medicine in the division of renal diseases at Washington University School of Medicine in St. Louis. Stones form when your urine becomes concentrated and there’s not enough water to keep the urine dilute. Meat eaters are also prone to kidney stones because animal protein contains amino acids that are broken down into phosphoric and sulfuric acid, which are secreted in your urine, making it more acidic. “When the pH of your urine goes down, you’re more likely to form most stones,” Miller says.
Stone symptoms
Kidney stones are brown or yellow, and range in size from a grain of sand to a golf ball. The edges may be smooth or uneven. Stones that are smooth and small (less than 5 mm, about 0.2”) usually cause no problems. The exception is people with bleeding disorders. Marcella’s stones have all been around 2–3 mm (5/64”–1/8”). “Not that big, but for someone with hemophilia, they can cause serious trouble if they get in there and tear something,” he says.
Sizable, jagged-edge stones that travel use pain as their calling card. As smooth muscles strain to push them through the ureter, urine flow is interrupted, and pain and pressure build. Relive your worst stomach ache, a lengthy labor and delivery, or post-surgery pain. You haven’t come close to the knifelike pain in the back, flank or stomach from a stuck stone or one on the move. “I felt nauseous and had vomiting—the real nasty stuff,” Marcella says, recalling the pain from a stone in transit. Chills and fever can also come along for the ride.
Pain while urinating and blood in the urine are other symptoms. “Bleeding is fairly typical of a kidney stone,” says Miller. “Someone with hemophilia will notice the bleeding.” That’s true for Marcella, who’s had four kidney stones since he was 19. “The way I found out about the first one was I had hematuria, or blood in the urine.”
Help is on the way
Wavebreakmedia Ltd/ThinkstockWhether you end up in the ER or your doctor’s office, a few telling tests will be taken. Urinalysis shows if you’re battling an infection and what substances the stone contains. A blood test reveals if you have elevated levels of calcium phosphorus and uric acid. A CT scan or ultrasound can confirm the diagnosis.
For most patients, there’s a wait-and-see approach. They’re given pain medications, encouraged to hydrate and sent home to let the stone pass on its own, usually within 24–72 hours, Miller says.
But stones that are large, painful or block the flow of urine need to be retrieved. Further grounds for immediate removal include an infected kidney stone or if you have only one kidney, to prevent it from becoming obstructed, says Miller.
The most common procedure is shock wave lithotripsy, which pulverizes the stone with pulses of shock waves. However, it is not recommended for people with bleeding disorders because it could produce muscle or joint bleeds, warns Miller.
Instead, you may undergo a ureteroscopy at the hospital. “This would be the preferred procedure for someone with hemophilia because it’s in a controlled setting where you can dose factor,” says Miller.” A ureteroscope is a long, tubelike device with a lens or digital camera and a light on one end, and an eyepiece on the other. Once the stone is located, the urologist retrieves it with a tiny wire basket or breaks it up with a laser.
A third method which is used occasionally, is percutaneous nephrolithotomy. A nephroscope, a hollow tube inserted through an incision, locates and removes the stone. It is employed when the stone is large or irregularly shaped, or if part of it still remains after lithotripsy.
It’s important to coordinate communication between your urologist or nephrologist, hospital and hemophilia treatment center (HTC) team. The hospital staff needs to know how to manage your bleeding disorder before and after a kidney stone procedure. “People would need to have their factor level higher than they typically would,” Miller says. “Then they would treat afterward, just like any other invasive procedure.”
The wonders of water

Serezniy/ThinkstockA solution may be as close as your faucet. Water in high enough quantities can prevent kidney stones from forming, says the American College of Physicians (ACP). That and other evidence-based guidelines were published in the Annals of Internal Medicine in 2014.
The two most common ways to stay stone-free are to pump the fluids and tweak your diet. If those fail, some medications can help.
The 2014 ACP guidelines recommend drinking enough liquids to produce at least 2 liters (96 ounces or 12 cups) of urine daily. Water is your best bet. But lemonade and limeade are also beneficial. They contain high levels of citrate, which helps prevent calcium from glomming onto other substances that form stones.
“I try to drink about two liters per day,” Marcella says. “I try to stay hydrated with water and drinks with electrolytes.” He stays away from energy drinks and colas these days. Dark sodas contain phosphoric acid, which can contribute to kidney stone formation.
Revamping your diet
You may be told to avoid foods containing purines, chemicals that are broken down into uric acid. Purine-rich foods include organ meats, red meat, some types of seafood and beer.
Sodium, a component of salt, causes your body to lose calcium in your urine, increasing its saturation and causing the formation of more stones, says Miller. “No one in the US eats a low-sodium diet. I always say eat a lower- or normal-sodium diet,” he says. Stay away from salty foods like canned soup and soy sauce.
If oxalates cause your kidney stones, eliminate such offenders as rhubarb, spinach, beets, nuts and chocolate.
Even if your kidney stones are made of calcium, don’t banish it, the NKF says. Studies show that eating calcium-laden foods with oxalates binds them together in the stomach and intestines, actually lowering your risk of kidney stone formation. “You want to be on a normal-calcium diet,” Miller says.
The ACP guidelines stated that when fluid therapy fails, some medications succeed. Thiazide diuretics, citrate and allopurinol all produced statistically significant results in preventing kidney stones.
Marcella has taken steps to revamp his diet. He now eats more citrus fruits and vegetables. Although a self-proclaimed “meat-and-potatoes kind of guy,” Marcella’s cut way back on red meat, too. “I want to eliminate the possibility that my intake is causing the stones.”
Plan ahead
Still, kidney stones can recur. Without preventive measures, kidney stones return in up to 50% of people within five years, says the NIDDK. “Work with your urologist or nephrologist to prevent recurrence and have a plan,” says Miller. Talk to your HTC staff to create a treatment plan before you land in the ER with another stone. “You don’t want to just leave it to chance,” he says.

