Ah, that oh-so-familiar scenario: Your ankle is tingly, feels warm to the touch and hurts. It’s a joint bleed—or is it? “These symptoms are nonspecific and can occur with any kind of arthritic or acute inflammatory condition,” says Annette von Drygalski, MD, PharmD, director of the Hemophilia and Thrombosis Treatment Center at the University of California San Diego (UCSD). In a 2013 study in Haemophilia on patients with hemophilia, von Drygalski and colleagues found that patients’ perceptions of the cause of their pain were correct only one-third of the time. And their doctors’ diagnoses, based on physical exam and patient interviews, were correct less than half the time. “There are many reasons why someone could have a swollen, painful, hot joint,” she adds.
To help differentiate the source of patients’ pain and swelling, von Drygalski is on a crusade to promote musculoskeletal ultrasound (MSKUS). Her center is the only one in the country holding trainings for hemophilia treatment center (HTC) staff to learn how to use it. The timing could not be better, as patients are lining up for the procedure. “Patients call in all the time to get their joints scanned,” says von Drygalski. She sometimes performs four or five ultrasounds per day. “MSKUS has revolutionized how we diagnose joint bleeds and disease.”
Before calling your HTC to find out if and when it will start using MSKUS, learn more about what it is, what it does and what limitations it has.
Understanding ultrasound
Ultrasound, or ultrasonography, is the use of sound waves to provide medical information. It’s been used for medical imaging of everything from fluid-filled cysts to the growing fetus in a mother’s womb. Although new to hematology, MSKUS has been a standard practice in orthopedic medicine and sports medicine for years.
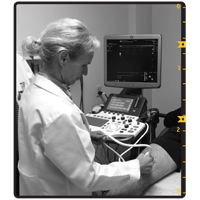
Photos courtesy of Annette von Drygalski, MD,
PharmD, Hemophilia and Thrombosis Center,
University of California San Diego
Dr. von Drygalski performs MSKUS
on a knee joint.
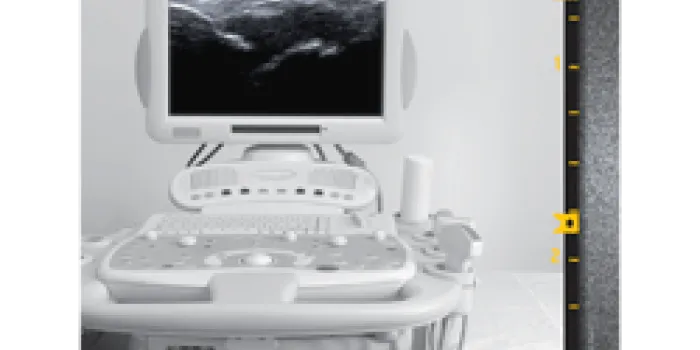
To take images of a joint, a probe called a transducer is gently moved over the area. A gel is applied to the skin to help the transducer glide better and decrease distortion. Shaped like a hockey stick or computer mouse, the transducer emits high-frequency sound waves that bounce off structures in the joint and are reflected back. The transducer converts these echoes into electrical signals that appear as images on a screen.
With the latest advancements in technology, ultrasound machines now have flat screens or touch screens, and sophisticated software. Some are portable, making it easier to wheel them from room to room. With the advent of smaller, more sensitive transducers, ligaments and tendons are now visible. MSKUS can even document changes in cartilage resulting from osteoarthritis and synovitis, chronic inflammation of the synovial membrane surrounding the joint. When combined with power Doppler, MSKUS can detect inflammation and abnormal blood flow. “It’s been a great tool to confirm hypervascularity (increased blood flow), a hallmark of synovitis,” von Drygalski says.
The real test of MSKUS is its ability to confirm the presence or absence of blood in a joint. “It is a bit tricky, but there are published criteria to distinguish bloody from nonbloody,” says von Drygalski. “It’s a speckled gray appearance of compressible matter.”
Tendon and ligament injuries lend themselves to MSKUS imaging. “You can distinguish how much has ruptured or how much the fibers have been disturbed, from partial- to full-thickness tears,” von Drygalski says. In a 2015 study von Drygalski co-authored in Haemophilia, MSKUS picked up undiagnosed tears and sprain in about 10% of the scanned joints.
Learning curve
Since February, UCSD has been hosting almost monthly 3-day hands-on training courses with continuing medical education credits. “We did that due to an incredible demand from other physicians, HTCs and providers to learn this,” von Drygalski says. The course is hemophilia-specific and includes instruction on measuring synovial growth, cartilage damage, tears and sprains. “This is a different use of the ultrasound, diagnosing the etiology (cause) of acute pain vs. assigning scores for joint health,” she says.
So far, students have come from Canada, Los Angeles, Pennsylvania and Washington, to learn MSKUS. Among them is Cindy Bailey, PT, DPT, OCS, SCS, physical therapist at Orthopaedic Hemophilia Treatment Center (OHTC) at the Orthopaedic Institute for Children in Los Angeles. She’s taken the training course twice, the second time to establish standards of operator reliability. “Once you’ve been trained to see it, you can pick out very delicate differences,” she says. “I could see the synovitis, with the synovial fringe hanging down into the joint capsule.” Fluid was also distinguishable. “If it’s old, it shows up as a speckly white. It displaces when you put pressure on it with the transducer head,” she says. “If it’s new or from an inflammatory process, then it’s clear.”
At least one student was not so gung-ho on the ultrasound procedure at first. “I was a very big skeptic when Dr. von Drygalski first brought it up,” says Doris V. Quon, MD, PhD, medical director at OHTC. But after taking one course, she’s changed her mind. “I think it would help the patients, and that’s most important.”
Wavebreakmedia/ThinkstockMSKUS has advantages over MRI, including the speed with which results are ready. “If you’re the ultrasonographer, you can get your answer immediately,” remarks Quon. Its sensitivity is also a plus. “MRI is not as sensitive as MSKUS to soft tissue changes and bleeding,” von Drygalski says. And patients appreciate the comfort factor. “It’s not like an MRI, which is noisy and annoying,” says John Powers, 38, who has severe hemophilia A. “They had the lights off and I was lying down on a bed. It was relaxing,” says the information technologist from San Diego. When time matters, MSKUS delivers. A full joint exam using MSKUS takes 10–20 minutes; an MRI can take three to six times longer. (See sidebar, “MRI and MSKUS Go Head to Head.”)
Limitations
Both the trainers and students of MSKUS admit it has limitations. “The drawback is that it cannot go to the interior of the joint,” says von Drygalski. For instance, MSKUS can’t detect an anterior cruciate ligament tear in the knee, she says. It cannot penetrate bone, and images may be compromised in patients who are obese. Quon is not convinced that MSKUS is foolproof in pinpointing the source of pain. “Even if fluid is present, that doesn’t mean it’s blood,” she says. She acknowledges that there are ways to distinguish blood from a joint effusion, or fluid. “But it won’t do it 100% of the time.”
And, as with all technology, practice and expertise make perfect. “It will be very physician-dependent,” Quon says. Bailey is the PT at her HTC. “She knows the anatomy better than I do in terms of muscle groups, so she’ll pick it up faster.” Lastly, the cost may be prohibitive for smaller centers or clinics.
The proof is in the patients
For the skeptics, MSKUS is initially theoretical until it is used on patients in the clinic. The UCSD course lets students work on actual patients who call the HTC to have their joints scanned. Bailey scanned one patient’s elbow. “We were able to see in an old elbow bleed that all of the fluid in the joint had not resolved, although he had no pain,” she says. Suddenly, the man’s weekend plans changed. Instead of packing the car and heading to the beach for an afternoon tossing a Frisbee® with his kids, he decided to ice his elbow, wrap it and let someone else do the heavy lifting. “For him, it was an eye opener that he needed to take it easy,” says Bailey.
In contrast, another patient was sure he had blood and fluid in his ankle joint. “We, as the students, couldn’t find anything—no blood or inflammatory fluids,” admits Bailey. But neither could the instructor. A cortisone injection improved the man’s symptoms, which were caused by inflammation, she says.
Powers has had several joint bleeds imaged by MSKUS. “They could see where the bleeding was exactly and they prescribed my factor differently,” he says. Until then, he typically treated a spontaneous bleed with a double dose of clotting factor that day, that night and the next morning. “I was putting myself at risk for a clot,” Powers says. “It was very dangerous.” Instead, his hematologist prescribed a smaller dose of clotting factor over a longer period. She then re-examined his joint using MSKUS to see if the bleed had resolved.
The results from Powers’ MSKUS scans have improved not only his treatment regimen, but also his exercise routine. He has stopped lifting heavy weights and started lighter exercises. “I’m more prone to do physical activity that helps prevent the knee from deteriorating faster,” says Powers. “I’ve changed my behavior in a positive way. Hopefully, it will make my joints last longer.”
Because MSKUS offers what’s called “point-of-care” service, patients no longer have to make an appointment in the radiology department, be imaged by a stranger and wait for results. Instead, their hematologist or PT can perform the ultrasound in the exam room and share the experience. “I have a doctor telling me exactly what is what on the screen,” says Powers. “Sometimes I look at it, and I can’t believe that’s my body.” He feels more involved in the whole process. “I’m following a story and I’m part of the story.”
And that story no longer has to be a mystery with sketchy clues, thanks to the immediacy of MSKUS. “The point-of-care decisions the doctor will be making with our information from the ultrasound will change the landscape for the patients,” Bailey says.
Joining the ranks
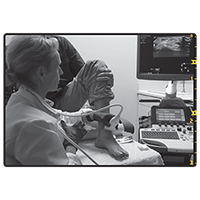
Dr. von Drygalski moves the transducer
around while performing MSKUS
on an ankle.
OHTC staff are anxiously anticipating how they will use their new MSKUS equipment. First, they will record baseline measurements of all their patients’ elbows, knees and ankles. That way, they can see any changes over time, says Bailey.
The use of the ultrasound technology is a potential win-win for both patients and their doctors. There’s the education component. “We’re hoping to help our patients distinguish the difference between the pain of having a bleed and the pain of having some arthritis or tendinitis changes,” Bailey says. For the patient who’s convinced every pain is a bleed, MSKUS will clearly show otherwise. “I’ve tried to explain that this is arthritis,” Quon says with a hint of frustration. “This will provide additional evidence for this type of patient.”
For patients who scoff at treatment because they’re used to living with arthritis, MSKUS will also persuade them. “You can show them that there’s a lot of fluid along these borders and the joint has telltale signs of being a bleed,” Quon says. Their clotting factor dosage can then be modified accordingly, she says.
Yet other applications for MSKUS exist. One is called guided imagery, using the technology for more precise placement of a cortisone injection, for example. “Your accuracy rate goes from a range of 42%–91% without it to 90%–99% with it,” Bailey says. MSKUS can direct the aspiration of fluid or blood from a swollen joint. “You feel more comfortable doing it because you actually see where you’re going in real time,” Quon says. And PT plans will be revised by MSKUS. By having a patient move a limb to the point of pain, Bailey will use the ultrasound to detect sharp edges on bones or swollen tendons, inhibiting gliding. “It will help us plan how aggressive to be and in what ranges of motion,” she says.
Quon pictures using MSKUS proactively and preventively in children during their annual HTC visit. “If they have signs of arthropathy (joint disease), then we can become more aggressive with their prophylaxis to prevent further arthropathy,” she says.
Joint longevity
Powers is taking part in a clinical study of MSKUS. “As I go through the study, I’ll find the best approach for my prophylaxis and how to adjust it,” he says. His ultimate goal is simple: joint preservation. “I want to get more longevity with my joints.”