The patient weighed about 300 pounds, was 6 feet tall and had severe hemophilia A. His body mass index (BMI) was 40, 10 points above the cutoff for obesity, according to the National Heart, Lung, and Blood Institute (NHLBI). His weight was putting more pressure on his joints, contributing to frequent, spontaneous bleeds in his knees and ankles that later led to joint disease.
“He was able to get around, but he was in significant pain,” recalls Mindy Simpson, MD, a pediatric hematologist at the Rush University Hemophilia and Thrombophilia Center in Chicago. The most disturbing part for her: The young man was only in his 20s.
“These types of complications are becoming more common,” Simpson says. “Even though there’s so much acceptance that ‘oh well, children are just heavier than they were 20 years ago,’ it’s not something that we can ignore.”
Obesity is a worsening public health problem among the general population and the bleeding disorders community. But medical experts and NHF are working to change that.
Obesity on high alert
Obesity is different from other chronic medical issues. Unlike hemophilia, where there’s an immediate medical protocol that must be followed, obesity can be easily dismissed. Further, many parents are in denial. More than half underestimate their obese or overweight child’s weight, especially if the child is between 2 and 5 years old, according to a February 2014 study in the journal Pediatrics.
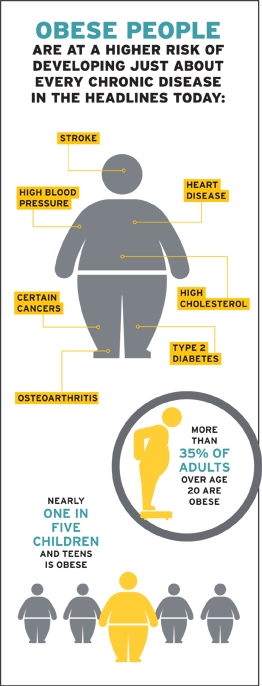
Not recognizing the problem means not dealing with it. The reluctance to address obesity could be the reason it’s becoming a national epidemic. Between 1980 and 2008, obesity rates doubled for adults in the US. During that same period, rates for children tripled, reports the US Centers for Disease Control and Prevention (CDC). The statistics are alarming: More than 35% of adults over age 20 are obese, and nearly one in five children and teens is obese, according to CDC figures from 2012.
But the real problem with obesity is that it’s like a storm warning, signaling that other medical conditions are looming. Obese people are at a higher risk of developing just about every chronic disease in the headlines today—type 2 diabetes, heart disease, high blood pressure, stroke, high cholesterol, osteoarthritis and certain cancers.
In June 2013, the American Medical Association (AMA) raised the national alert about obesity by declaring it a disease. “Recognizing obesity as a disease will help change the way the medical community tackles this complex issue,” said AMA board member Patrice Harris, MD, in a press release announcing the decision. In other words, doctors and patients need to start taking it seriously.
One issue on top of another
Obesity rates among people with hemophilia are on par with the general population. CDC data from 2005 found that 34.5% of hemophilia patients age 20 and older were overweight. More than 23% were obese, according to a December 2011 study in the American Journal of Preventive Medicine.
Data from a study by Ed Kuebler, LCSW, social worker for the Gulf States Hemophilia & Thrombophilia Center in Houston, gave even higher estimates. About 38% of youth and 59% of adults with hemophilia were overweight or obese.
The difference is that people with hemophilia often experience the consequences of excess pounds immediately, usually in the form of joint limitations and bleeds, like Simpson’s patient.
That’s because being overweight or obese speeds up the loss of joint mobility for people with hemophilia, reports a March 2011 study in the journal Haemophilia. It also leads to more frequent joint bleeds, which lead to joint disease, which leads to even more bleeds, and so on in a continuous loop. “The joints have to bear more weight, which increases the amount of work they do on a daily basis,” Simpson explains.
In addition to joint disease, type 2 diabetes is also particularly concerning for people with hemophilia. Managing type 2 diabetes often involves insulin injections, which could lead to more bruising, Simpson notes. People with diabetes can experience poor wound healing, especially on their feet and legs. Hemophilia already makes wound healing a challenge. The worst-case scenario happens when diabetic foot ulcers lead to amputations.
Obesity’s other costs
Michael Recht, MD, PhD, was one of the authors of the 2011 Haemophilia study that cited the high obesity rates among people with hemophilia. “If you look at data over the last 10 years, what we’ve seen is that obesity rates are increasing faster among people with hemophilia than in the rest of the US population,” he says.
As medical director of the Oregon Hemophilia Treatment Center in Portland, Recht is also seeing obesity create additional challenges for his pediatric patients. One of those challenges is factor use. “If kids are really overweight or obese, it’s difficult to access their veins to give factor,” Recht explains. This could be why overweight and obese men and teens are less likely to perform home infusions or self-infusions than normal-weight men, according to a May 2014 study in the journal Haemophilia.
For the family, obesity also means additional costs. An obese child already chalks up an additional $19,000 in lifetime medical costs compared with a normal-weight child, according to an April 2014 study in the journal Pediatrics. Because factor is diagnosed based on current weight, not ideal weight, families end up with higher healthcare costs for factor when their affected children are overweight or obese.
Then, there’s the social torment of being an obese kid with hemophilia. “We know that children with special healthcare needs have a harder time at school and interacting with peers,” Recht says. “If they feel different already because they have hemophilia, they now have the added stigma of being overweight or obese.”
Simpson’s young patients also struggle with social issues, from poor school performance to self-esteem issues and depression. “Puberty is a tough time anyway,” Simpson says. “We’re seeing social isolation and depression-type symptoms. Kids who used to be straight-A students now have performance issues.”
But addressing all the problems obesity can cause is not enough. “To me, the issue is why are our patients obese, and what can we do to prevent it?” Recht says.
Prevention: Eat right and exercise

bubaone/Thinkstock
Recht’s study drew the same conclusion as most other studies on obesity: “Simple steps can be taken to encourage patients to decrease caloric intake and increase physical activity,” he says.
The CDC recommends 6- to 17-year-olds get at least an hour of moderate to rigorous aerobic activity every day. That includes muscle- and bone-strengthening activities at least three days each week. Adults should get about 150 minutes of moderate aerobic activity or 75 minutes of high-intensity aerobics each week, says the CDC. That should include muscle-strengthening activities at least two days a week.
In addition to regulating weight, exercise can also improve mental health, reduce the risk of heart disease and certain cancers, and increase life expectancy, according to the CDC. Before starting an exercise program, check with your hemophilia treatment center (HTC) team about which exercises are appropriate.
The overall goal of the dietary changes is to reduce salt, cholesterol, fats and added sugars, and increase the variety of fruits and vegetables eaten every day. These recommendations are given in the US Department of Agriculture’s (USDA’s) 2010 Dietary Guidelines for Americans, which are slated to be updated in 2015.
The steps to increase exercise and improve diet may look simple, but they are not always easy. For example, Recht has found that food insecurity is one of the primary drivers of poor eating habits among his obese patients with hemophilia. “They don’t know if they’ll have enough for food for the month,” he explains. “Less healthy food is less expensive.”
Recht’s HTC is addressing this issue by working with a nearby farmer’s market. He can write his patients a prescription for fruits and vegetables, and families can shop at the farmer’s market for free.
Taking control

Digital Vision/Thinkstock
Eating healthy and exercising regularly start with noticing the environmental barriers that make an obese person’s surroundings “obesogenic,” says Tania Heller, MD, FAAP, medical director of the Washington Center for Eating Disorders and Adolescent Obesity in Bethesda, Maryland.
Temptation comes in the form of having too much food available. “Food is around 24/7, including snacks and sugary drinks,” says Heller, who presented the session “The O Word: How to Think About Obesity in a Patient-Centered Way,” at NHF’s Annual Meeting in 2014. “Families who eat out a lot may think their meals at home should mimic the supersized portions they eat in restaurants,” she adds.
Overeating is then combined with the average of 7.5 hours a day young people spend doing sedentary activities like watching TV or chatting on social media, according to a January 2010 study by the Kaiser Family Foundation, a nonpartisan public health think tank. That’s more than three times longer than the two-hour block of screen time recommended by the American Academy of Pediatrics to prevent obesity. If children are spending the equivalent of a full-time job in front of a screen, they are not getting adequate physical activity to stay healthy.
Heller’s medical team coaches families on how to deal with obesity by making overall lifestyle choices. “I don’t talk too much about calories and numbers with young people,” Heller cautions. Instead, she helps people find their motivation. Maybe it’s avoiding joint bleeds or socializing with friends. Whatever it is, that motivation has to stay top of mind in order for healthy lifestyle changes to become healthy habits, Heller says.
The next step is to work with the HTC medical team to set safe, appropriate goals for the desired actions, not the numbers on the bathroom scale. “Instead of saying, ‘My goal is to lose 10 pounds,’ say, ‘My goal is to walk 30 minutes a day this week,’ ” Heller says.
Several online apps help people track their daily food intake and exercise regimen. For example, the USDA’s free SuperTracker can help with online meal planning, food journaling, and setting personal goals like calorie intake and physical activity targets. The website launched in December 2011 as part of first lady Michelle Obama’s nationwide fitness initiative, Let’s Move, according to a USDA press release. By September 2012, the site boasted its millionth user.
Even with online tools and personal motivation, weight management can still suffer if the home environment isn’t supportive. That means families need to be careful how they address obesity with their children. “Try not to make the conversation about weight and numbers, but about strength of character and accomplishments,” Heller says. “Too many children get teased at school. Home should be a safe haven.”
Joining the nation’s fight
For families affected by hemophilia, embracing regular exercise means clearing up any pervasive myths about how people with bleeding disorders should not engage in physical activity.
In October 2014, NHF and CDC launched a cooperative agreement to create health education programs to reduce joint disease. “The bleeding disorders community needs more information and programs to encourage safe physical activity,” says Ayana Woods, NHF’s director of education. “To improve joint function and overall wellness, we need to educate children and adults about the importance of exercise and prophylaxis.”
The five-year initiative will include online and offline components: a monthly webinar series developed by physical therapists and nurse-led workshops. NHF will supplement these programs with bilingual print materials, and videos for children and parents whose first language is Spanish.
The initial step, however, is to do a nationwide needs assessment among the bleeding disorders community to identify barriers and misconceptions about exercise and treatment. “This national public health initiative that encompasses chapters, HTCs and community members has the potential to not only improve joint function in people with bleeding disorders, but also move us one step closer to ending the obesity epidemic,” Woods says.
filmfoto/Thinkstock

