When Barbaro, the 2006 Kentucky Derby winner, shattered multiple bones in his right hind ankle two weeks after the race, it was a grim reminder of the consequences of constant pounding on thoroughbreds’ joints. Like horses, the ankles of humans bear the body’s weight and are the site of sprains, strains and breaks. For people with hemophilia, ankles are one of the target joints, prone to repeated bleeds. If untreated, they can develop arthritis or joint disease, which significantly limits range of motion and affects quality of life.
“Both my ankles have been my number one target joint since childhood,” says Victor Miranda, 25, of Ontario, California. “I had so many ankle bleeds. I remember being on crutches or using a walker. It cost me days from school.”
Miranda, a warehouse worker, didn’t consider surgery until he was 23. Now he’s undergone ankle fusion surgery in both ankles. “Before my surgery, just walking an hour or two—that was it for me, I had to rest,” he says. “I was limping because of all the pain in there. I had to take some kind of medication for the pain.”
But once he had the surgery, things changed dramatically. “When I wake up my ankles aren’t stiff,” says Miranda. “Now I’m able to work my eight-hour shift. It’s just a complete turnaround.”
The decision to have ankle fusion surgery usually comes after years of ankle bleeds, arthritis, loss of mobility and, ultimately, unbearable pain. But the degradation of the ankle can start early on—with the first bleed, which can occur in early childhood. However, ankle bleeds are not inevitable in this day and age. Prophylaxis can help stave off joint bleeds, helping prevent long-term destruction of the ankle joint and other joints as well. (See NHF’s Medical and Scientific Advisory Council’s[MASAC] Recommendation #102, which calls for further data collection from currently available treatments, as well as MASAC Recommendation #179, concerning prophylaxis.)
[Steps for Living: Treat Responsibly Today for a Healthy Tomorrow]
Treatment options for chronic joint disease in the ankle include chemical or surgical synovectomy (removal of the synovial lining of the ankle) and ankle fusion or ankle replacement surgery. To understand these treatment options, it is important to understand the anatomy of the ankle and what happens to it over time in a person with chronic ankle bleeds.
Ankle Anatomy
The ankle joint is composed of three bones—the tibia, or shin bone, the large bone of the lower leg; the fibula, the small bone of the lower leg; and the talus, the large bone of the foot. Ligaments support the joint, providing stability. Tendons and muscles move the ankle and foot. The ankle is a hinged joint with movement in two directions: toward the body, which is called dorsiflexion, and away from the body, which is called plantar flexion. It is the weight-bearing joint of the foot and acts as a shock absorber.
Bleeding into the ankle can wreak havoc with the mechanics of the joint. “Blood is not a normal component of the joint,” says Mauricio Silva, MD, orthopedic surgeon at Orthopaedic Hospital in Los Angeles, and assistant professor in the department of orthopaedic surgery at the David Geffen School of Medicine at the University of California, Los Angeles. “When it accumulates in the joint, it destroys the cartilage through two different mechanisms—directly and indirectly, by inducing an inflammation of the synovium, which can release enzymes that secondarily destroy the cartilage as well.”
The synovium is a thin membrane lining the ankle joint. With repeated bleeds, the synovium becomes inflamed and irritated from the continual deposit of iron from the blood. Chronic inflammation is called synovitis, characterized by a thickened synovial membrane with an expanded bed of capillaries, which are prone to bleeding. A pattern then develops of frequent bleeding into the ankle, ongoing cartilage destruction, bone damage and the development of arthritis, which can cause disability and deformity.
“If hematologic management fails, the first surgical procedure we do around the ankle is usually synovectomy [through a small incision in the joint],” says Marvin Gilbert, MD, orthopedic surgeon at The Mount Sinai Hospital in New York. He is also founding co-director of the International Hemophilia Training Center and clinical professor of orthopedic surgery at the Mount Sinai School of Medicine. “It’s almost always done arthroscopically, the risks are not great and the results are fairly satisfying—it stops the bleeding and controls swelling.” As far as arthritis goes, the surgery can only temporarily arrest it, he says.
Arthritis in the ankle can cause tenderness in the front of the joint and limit range of motion. Gilbert says X-rays of the joint often reveal the presence of osteophytes, small bony projections at the edge of an arthritic joint. “By arthroscopically removing the spurs from the front of the joint, it will frequently stop some of the pain and return some of the lost motion,” says Gilbert. Arthroscopy is a minimally invasive surgical procedure in which small incisions allow the insertion of an endoscope in the joint. “But if that doesn’t work, you have to consider an ankle fusion.”
The Fusion Decision
Most ankle fusions, or arthrodeses, are done on men between the ages of 20 and 50. Although some teens have had them, it is usually not recommended. Growth plates at the ends of bones continue to add length and height as a young adult grows. Performing the surgery too early could stunt growth, causing a leg length difference.
The surgical solution becomes viable for most people when their quality of life is affected by intolerable pain and loss of mobility. But the decision to go through with an ankle fusion is frequently preceded by procrastination. Fusion is often equated with no motion. “People are very reluctant to have the surgery because they think it’s going to disable them,” says Gilbert. “Interestingly, at the ankle, it doesn’t.”
By the time Miranda was a senior in high school, his right ankle had become a problem. It was stiff when he woke up. He had to warm it up just to get moving. If he sat for long periods, it would become stiff all over again. “I was about 20 when my doctor first suggested ankle fusion surgery,” says Miranda. “I wasn’t really into it at first because I was afraid I wouldn’t be able to walk the same way.” He waited three years before he had his first ankle surgery in April 2005.
Gilbert says that by the time most people undergo fusion surgery, they probably have little to no motion in the ankle, but don’t realize it. “They think they’re having some motion, but that happens to be motion in the bones below the ankle, which allows the foot to look as if it’s going up and down and in and out,” says Gilbert. “They think they’re having tibiotalar (true ankle joint) motion; what they’re really having is subtalar motion (movement of the joint below the talus bone).”
The Surgical Procedure
The typical fusion in the ankle occurs between the tibia and talus joints and is called tibiotalar fusion (although subtalar fusions are also done when needed). In the arthroscopic procedure, the surgeon removes the remaining cartilage on the talus and tibia, exposing the bones, and then aligns them for proper fusion. “You then have two raw ends of bones,” says Gilbert. “The body identifies it as a fracture and determines to heal it. So the bones fuse together.”
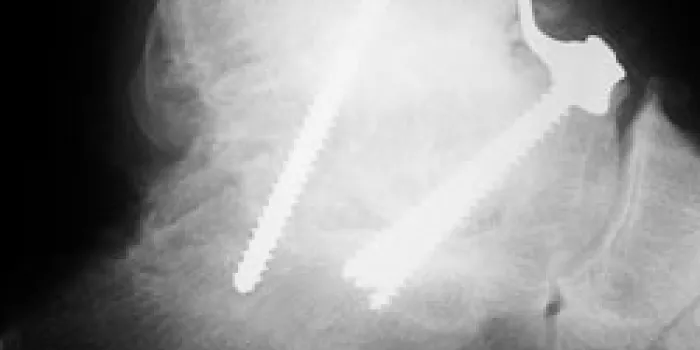
Although there are many methods used, typically metal screws, pins, plates or rods are put in place to anchor the joint until it heals. In a crossed screw fixation, one goes diagonally through the tibia on the inside, the other diagonally through the fibula on the outside into the talus to hold it. A cast keeps the ankle immobilized while the bones fuse, protecting the joint. Most patients are in the cast for six weeks without bearing weight on it. After that, the cast is removed and the patient is in an ankle brace, commonly a boot with Velcro® straps, bearing weight on it while on crutches for another six weeks. In most cases, 12 weeks is the minimal amount of time needed for healing. Full recovery and returning to activities can take up to nine months, depending on the patient.
Post-op and PT
Once the cast is removed, some physicians recommend physical therapy (PT) for their patients. “If everything is fine on the X-ray and looks healed, I refer people to PT because they need to be retrained on how to walk,” says Silva. “Range of motion is not our concern anymore, because we took that away with the surgery. What the patient needs is strengthening exercises for the muscles around the ankle. After being in a cast for so long, those muscles are quite atrophic.”
“Changing the bones of a joint isn’t all there is to the procedure,” says Ruth Mulvany, MS, PT, at the University of Tennessee, Memphis. “You’ve got to rehab the muscles and soft tissues and the other joints that are also affected.”
It comes down to good biomechanics, Mulvany says—helping someone regain good posture and joint alignment. “If a person has walked abnormally because of an ankle problem, then the knee and hip also have problems,” she says. “We try to rebalance the muscles.” That might mean stretching the hip flexors or lengthening calf muscles that have become shortened over time as a result of an abnormal gait caused by chronic ankle bleeds. In addition, the patient might need to wear orthotics, custom-made shoes, braces or splints.
Some of the exercises are done at the clinic with the physical therapist; others are done by the patient at home. “Rehab takes a lot of commitment to be successful. It can take weeks or months,” says Mulvany. “For the patient at home, it might involve wearing a splint at night, doing stretches two or three times a day and adding strengthening activities. It’s not a quick fix.”
Complicating the Situation
All surgeries carry risks, but some are higher for people with bleeding disorders. Complications that can develop after ankle surgery range from arthritis to nonunions.
“You always pay for something when you fuse a joint,” say Gilbert. “A patient can develop arthritis in the subtalar joints on that same side because of the increased stress on them.”
Nonunions result when the bones do not grow together properly. “When you have bone-on-bone contact, bone cells usually grow them together, creating the fusion, but occasionally that doesn’t happen,” says Silva. “Instead, there are areas on the X-rays where we can see [lucencies]. It happens in the tibiotalar joint, but more commonly at the subtalar joint.” In most cases, there are no symptoms and no pain. “If pain appears, we can revise the fusion and re-fuse it,” he says.
Silva says that during the past 20 years, the rate of nonunions at Orthopaedic Hospital in Los Angeles has dropped from 50% for the subtalar joint to 22%, a rate he still considers somewhat high. “This is probably due to surgical techniques,” he says, which are improving all the time. “We are not quite at the point where I can say there will be no complications.”
Ankle Replacement Surgery
Ankle replacement surgery, or arthroplasty, is usually not recommended for someone with hemophilia. Although hip and knee replacements are routine now, ankle replacements are not. The reasons vary, but one of the main ones is the structure of the joint itself.
“The ankle has a very small surface area. All of your weight is distributed onto that small surface area; therefore, the forces there are very high,” says Gilbert. “In addition, there’s not a lot of padding around the joint. If you have a bleed, it really stresses the skin and soft tissues.” He says that ankle replacements at The Mount Sinai Hospital, where he works, are reserved for people with rheumatoid arthritis or who are relatively sedentary and will not place much stress on the new joint—to date, none of the candidates have had hemophilia. Gilbert does not perform ankle replacement surgeries.
“The first generation of ankle arthroplasties had a lot of complications, including infection, loosening and osteolysis (bone loss),” says Silva. Although second-generation arthroplasties are better, the follow-up has only been about five years, says Silva. “We have to wait until we have better evidence. In the future, we are going to have new ankle arthroplasty procedures that are good enough that we can take the risk and do them on our patients with hemophilia.”
Although ankle fusions are not perfect, Silva says, they do typically have good outcomes, and that’s why he prefers them. “Ankle fusion is still the gold standard,” he says.
New Ankles
After surgery, recovery and rehab patients anticipate what it will be like to walk with their ankle bones fused. “You would think that because of the ankle fusion, they wouldn’t be able to do anything afterward, but that is not true,” says Silva. “The patient can walk almost normally. I have seen patients who go back and play sports recreationally at the level they were at before surgery, but without pain. The results are quite good.”
“They told me that the surgery was going to take the pain away,” says Miranda. “As far as mobility, they said, ‘You’re going to be able to do more things than you can now.’”
Having had the other ankle fused in September 2006, he says those predictions have now come true. “I can pretty much say that I have new ankles,” Miranda says. Now married and working full time, he says he doesn’t even think about his ankles anymore. No longer limping or in pain, he also has had no further bleeds in either ankle.
“I’m happy with my results,” says Miranda. “To me, having both ankles fused was worth it. I feel good.”